American Indian and Alaska Native elders have long experienced disparities in health and healthcare. A health disparity is a preventable burden of disease, injury, or violence experienced by populations who have been subjected to disadvantages like discrimination in society.
Health disparities show the difference in health outcomes for different groups within the population. One such disparity is that on average American Indians die 12 to 13 years earlier than white Americans. Native people have higher death rates at most ages, but particularly at younger ages, and higher mortality for most of the top leading causes of death.
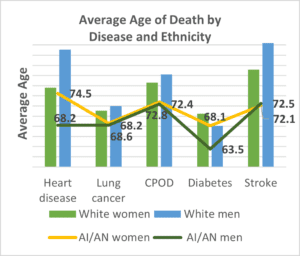 In 2018, the five leading causes of death for Native elders over age 65 were heart disease, cancer, chronic lower respiratory diseases, diabetes, and stroke.
In 2018, the five leading causes of death for Native elders over age 65 were heart disease, cancer, chronic lower respiratory diseases, diabetes, and stroke.
Social Determinants of Health
While it’s easy to focus on the numbers, the statistics represent the symptoms of the problem rather than the cause. The specific reasons for health disparities are complex and represent where people live and the services available and accessible to them. Factors such as having a regular source of care, language and communication barriers, lack of diversity in the healthcare workforce, high rates of poverty, lack of insurance coverage, discrimination against American Indians and Alaska Natives, and large distances from healthcare services have all added to the disparities that effect Native communities.
These factors are what the U.S. Department of Health and Human Services define as the “Social Determinants of Health.” Broadly, the factors fall into the following categories: economic stability, education, social/community setting, health and healthcare, and the neighborhood/environment. Disparities in Native health will not improve just by focusing on the numbers. Instead, improvement can be made through community health education, and economic standing, and by creating healthier and engaged communities.
American Indian and Alaska Native health disparities are symptoms of systemic problems. Six “Social Determinants of Health” are used to explain health outcomes, reduce risk factors, and implement systemic changes.
1. Income and wealth gaps
Native people can face greater challenges in getting higher paying jobs with good benefits due to less access to high-quality education, geographic location, language differences, discrimination, and transportation barriers.
2. Education
The historical trauma caused by the government relocation of Native children away from their families and tribal way of life to boarding schools created generational mistrust of educational systems. American Indians have the lowest educational attainment rates of any group in the United States. The approximately 180 Bureau of Indian Education schools are chronically underfunded, and while the majority of Native students attend public schools, they do not provide a culturally relevant curriculum or teacher training that promotes Indigenous history or identity.
3. Social/community setting
Centuries of racism in our institutional structures, policies, cultural norms, values, and individual behavior have impacted the places and relationships where Native people live, work, learn, play, and worship.
4. Health access and use
Many barriers to health care exist for people with disabilities, lower incomes, rural residences, and membership in a racial/ethnic group. Common barriers are lack of insurance, transportation, childcare, ability to take time off work, culturally insensitive patient-provider interactions, and inequities in treatment.
5. Neighborhood and physical environment
Native people residing in poor communities often lack access to public transportation, quality education, infrastructure (i.e. broadband), housing, affordable and nutritious food, jobs, and health care. Their communities may have higher crime, pollution, accident, and injury rates.
6. Workplace conditions
Some causes for work inequities are temporary work arrangements, lack of worker safety measures, limited or no health insurance benefits, and discrimination based on age, gender identity, race, and class.
 Historic and Contemporary Injustices on Native Health
Historic and Contemporary Injustices on Native Health
American Indian and Alaska Native populations have long experienced poorer health outcomes compared to other groups in America. The reasons are complex and connected to historic and ongoing racism, poverty, poor education, limited access to quality healthcare, forced relocation, and forced assimilation into non-Native culture.
Contemporary reasons for Native health differences include communication barriers, lack of diversity in the healthcare workforce, lack of insurance coverage, discrimination, and the need to travel long distances to hospitals and clinics for prevention, diagnosis, and healthcare services.
Indian Health Service (IHS)
The treaties negotiated between Native communities and the federal government established that tribes have a right to healthcare services. As such, the Indian Health Service (IHS) provides healthcare to over 500 federally recognized tribes. Because many tribes are seeking federal recognition, some Native people do not have access to IHS.
IHS services exist primarily in rural areas, yet approximately 70 percent of Native people live in cities and urban areas. Despite improvements in expanding healthcare and preventative services over the last 20 years, there is still a lack of hospitals and clinics on or near Native homelands.
What is Health Equity?
Health equity is when everyone has a fair and just opportunity to attain their highest level of health. It requires societal efforts to:
- Address historical and contemporary injustices
- Overcome economic, social, and other obstacles to health and health care
- Eliminate preventable health disparities
NICOA’s Commitment to Health Equity
Disparities in health are a major issue in American Indian and Alaska Native communities and stronger advocacy is needed to address these pressing needs. The National Indian Council on Aging (NICOA) strives to inform American Indian and Alaska Native elders and others about healthcare disparities so that there is greater understanding about the many factors that influence health statistics — especially those that impact Native communities.
As a National Center of Excellence, NICOA’s mission is to advocate for improved comprehensive health, social services, and economic well-being for Native elders. To help improve health equity among Native elders, NICOA supports policies that:
- Establish health education, awareness and prevention programs for Native elders
- Fund on-going research of health disparities in aging
- Improve health care access and quality for elders
- Promote inclusion of American Indians and Alaska Natives in gerontology and geriatric research
NICOA has created:
- Information and technical assistance for American Indian and Alaska Native communities to improve health care for Native elders
- An accredited curriculum for Native service providers
- Advocacy, education, and expert testimony when requested by Tribal Nations and the United States Congress
- Networks and partnerships to maximize resources and increase the efficiency and effectiveness of health service delivery systems for Native elders
 Historic and Contemporary Injustices on Native Health
Historic and Contemporary Injustices on Native Health